23-Year-Old Woman With Rare Blood Disorder Suffers Severe Reaction After Being Forced to Take Multiple Vaccines
Alexis Lorenze, who had abstained from vaccines due to religious reasons, faces life-threatening conditions after hospital mandated triple vaccination as condition for treatment.
Alexis Lorenze, a 23-year-old woman with a rare and life-threatening blood disorder, is in critical condition after suffering a severe reaction to vaccines mandated by UCI Medical Center as part of her treatment for paroxysmal nocturnal hemoglobinuria (PNH). Lorenze and her family had previously avoided vaccinations due to their religious beliefs. However, the hospital reportedly insisted that she receive three vaccines simultaneously as part of her medical care.
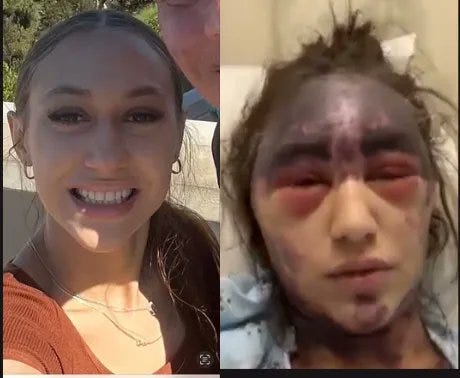
Newly surfaced photos and videos show the extent of Lorenze’s health deterioration, including significant damage to her ears, which may require reconstructive surgery. Lorenze’s condition has worsened since the initial report, and her family continues to seek answers about the necessity and safety of the vaccines administered. The story has sparked public concern and calls for accountability from the medical establishment involved in her care.
Despite Lorenze allowing the release of her medical records and giving permission for UCI Medical Center to discuss her case with FOX 11, the hospital has yet to respond to multiple requests for comment. The hospital has also not been clear on exactly which vaccines were administered, but they were likely to be tetanus, meningitis, and pneumonia vaccines.
A fundraiser to cover her medical costs, arranged by Steve Kirsch’s Kirsch Foundation, is at:
Ongoing live updates of Lorenze’s condition are available at CHD.TV.
What Is Paroxysmal Nocturnal Hemoglobinuria (PNH)?
Paroxysmal Nocturnal Hemoglobinuria (PNH) is a rare, acquired hematological disorder characterized by the destruction of red blood cells (hemolysis), leading to the release of hemoglobin into the urine, especially during the night or early morning. The condition arises from a mutation in the PIGA gene, which is responsible for the synthesis of a protein that helps anchor certain protective proteins to the surface of blood cells.
In PNH, the deficiency of these protective proteins (such as CD55 and CD59) makes red blood cells susceptible to destruction by the immune system, particularly by the complement system. This results in symptoms that may include:
Hemoglobinuria (hemoglobin in urine), often noticeable as dark-colored urine, particularly in the morning.
Fatigue and weakness due to anemia (low red blood cell count).
Abdominal pain and other gastrointestinal symptoms.
Thrombosis (blood clots), which can occur in various veins, leading to complications like stroke or organ damage.
PNH can occur as a standalone condition or in association with other bone marrow disorders, such as aplastic anemia or myelodysplastic syndromes. Diagnosis typically involves blood tests to detect abnormal red blood cells, flow cytometry to identify the absence of surface proteins, and sometimes urine tests.
Treatment options for PNH may include supportive care, such as blood transfusions or management of complications, as well as more targeted therapies. Eculizumab, a complement inhibitor, is one of the main treatments used to reduce hemolysis and the risk of thrombosis in patients with PNH. Other treatments include ravulizumab, an alternative complement inhibitor with a longer dosing interval.
Early diagnosis and management of PNH are crucial for improving outcomes and quality of life for affected individuals.
Lorenze was at UCI Medical Center to get treatment for her PNH; it is unclear why the hospital suddenly wanted to force multiple vaccinations on her as a condition of treatment.
Immune Thrombocytopenic Purpura (ITP) - A Known Vaccine Side Effect
Lorenze manifested a serious reaction to the three vaccinations within 10 minutes of injection.
According to MidwesternDoc, Lorenze’s lab tests showed that Lorenze had developed Immune Thrombocytopenic Purpura (ITP), an acknowledged yet rare side effect of vaccines. With ITP, the immune system targets its own platelets, which can cause serious clotting and bleeding issues throughout the body. Given that PNH makes blood cells more susceptible to attack by the immune system, it stands to reason that patients with PNH would be more likely to develop ITP following vaccination.
Despite the known connection between vaccines and blood clotting disorders, UCI Medical Center staff blamed the vaccine reaction on a Parvovirus infection, which was found to be positive in a PCR test.
Parvovirus, particularly Parvovirus B19, is primarily known for causing conditions like erythema infectiosum (fifth disease) in children and can lead to more severe complications in certain populations such as pregnant women, immunocompromised individuals, and people with chronic hemolytic anemia.
While Parvovirus B19 can lead to hematologic complications such as transient aplastic crisis and chronic anemia, there is no strong evidence directly linking it to blood clotting issues. However, any severe infection or inflammatory response (such as that stimulated by vaccine adjuvants) can potentially influence coagulation factors and platelet function indirectly.
Special Vaccination Instructions for Blood Disorder Patients
The question also remains as to why the hospital felt it would be safe to inject three vaccines at once in a patient with a pre-existing blood disorder, and whether they followed best practices.
When vaccinating patients with blood disorders such as hemophilia or paroxysmal nocturnal hemoglobinuria (PNH), several important considerations should be taken into account:
Factor replacement therapy:
Patients with hemophilia may require factor replacement before vaccination to prevent hematoma formation
For PNH patients on complement inhibitors, vaccines can be given within 24-48 hours of factor concentrate administration
Subcutaneous administration:
Some vaccines can be given subcutaneously instead of intramuscularly to reduce hematoma risk
This includes pneumococcal, polio, hepatitis A, and hepatitis B vaccines
Timing with treatments:
Patients on Emicizumab prophylaxis may not need additional treatment before vaccinations
Those on complement inhibitors should time vaccination close to their treatment dose
Avoiding live vaccines:
Live vaccines should be avoided in patients on high-dose steroids or immune-modulating drugs
This applies to those undergoing immune tolerance therapies or gene therapy protocols
Based on recommended best practices, it appears the doctors may have made several errors in administering these vaccines to a patient with a blood disorder like Paroxysmal Nocturnal Hemoglobinuria (PNH):
Simultaneous administration: Giving tetanus, meningitis, and pneumonia vaccines all at once may have been too aggressive for a patient with a bleeding disorder. The guidelines generally recommend spacing out vaccinations for such patients.
Lack of prophylaxis: For patients with blood disorders, especially those on complement inhibitors, factor replacement therapy or other prophylactic measures are often recommended before vaccination to prevent bleeding complications.
Intramuscular injection: The search results indicate that subcutaneous administration is preferred for patients with bleeding disorders when possible, to reduce the risk of hematomas. If intramuscular injection was used, this increased the bleeding risk.
Inadequate precautions: Guidelines recommend using a fine-gauge needle (23 gauge or smaller), applying firm pressure to the injection site for at least 2 minutes without rubbing, and monitoring for hematoma formation. These precautions may not have been followed.
Timing with treatments: For patients on complement inhibitors or other treatments, vaccinations should be timed close to treatment doses. This timing may not have been considered.
Lack of individualized approach: The patient’s specific condition, severity of PNH, current treatments, and bleeding risk should have been carefully evaluated before vaccination. A more tailored approach may have been necessary.
Insufficient monitoring: Close monitoring for adverse reactions, especially bleeding complications, is crucial for patients with blood disorders after vaccination. The massive reaction suggests inadequate follow-up.
These points highlight potential areas where the standard of care for vaccinating patients with blood disorders may not have been met.



This is horrible! So sad that with some simple research it should have been known that there were clear risks for giving a vaccine with her condition, let alone three at once. Someone needs to be fired for treating her like a pincushion. We are now a long way from "do no harm".